Consolidated billing
Consolidated billing: Financial precision, unified.

Managing premiums across multiple carriers, plans, and groups shouldn’t be a manual balancing act. As a core capability of the SIMON® platform, our consolidated billing engine integrates invoicing and premium payments into a single, high-performance financial workflow.
Instead of chasing reconciliation errors and juggling invoices, your team gains a unified billing system that handles the most complex benefit structures, turning multiple-carrier chaos into one clear, accurate process.
Universal Invoicing:
A single invoice across all plans and lines of coverage
Precision Disbursement:
Clean, accurate premium collection and disbursement
Zero Manual Reconciliations:
Eliminates manual reconciliation and multi-carrier complexities
Built for Complexity:
Built to support multiple employer organizations, participating groups, and diverse benefit offerings
Streamline your billing experience.
When enrollment, eligibility, and payments stay in sync, billing is easier to manage and to trust. SIMON keeps data aligned as changes occur, reducing rework and manual steps that slow teams down.
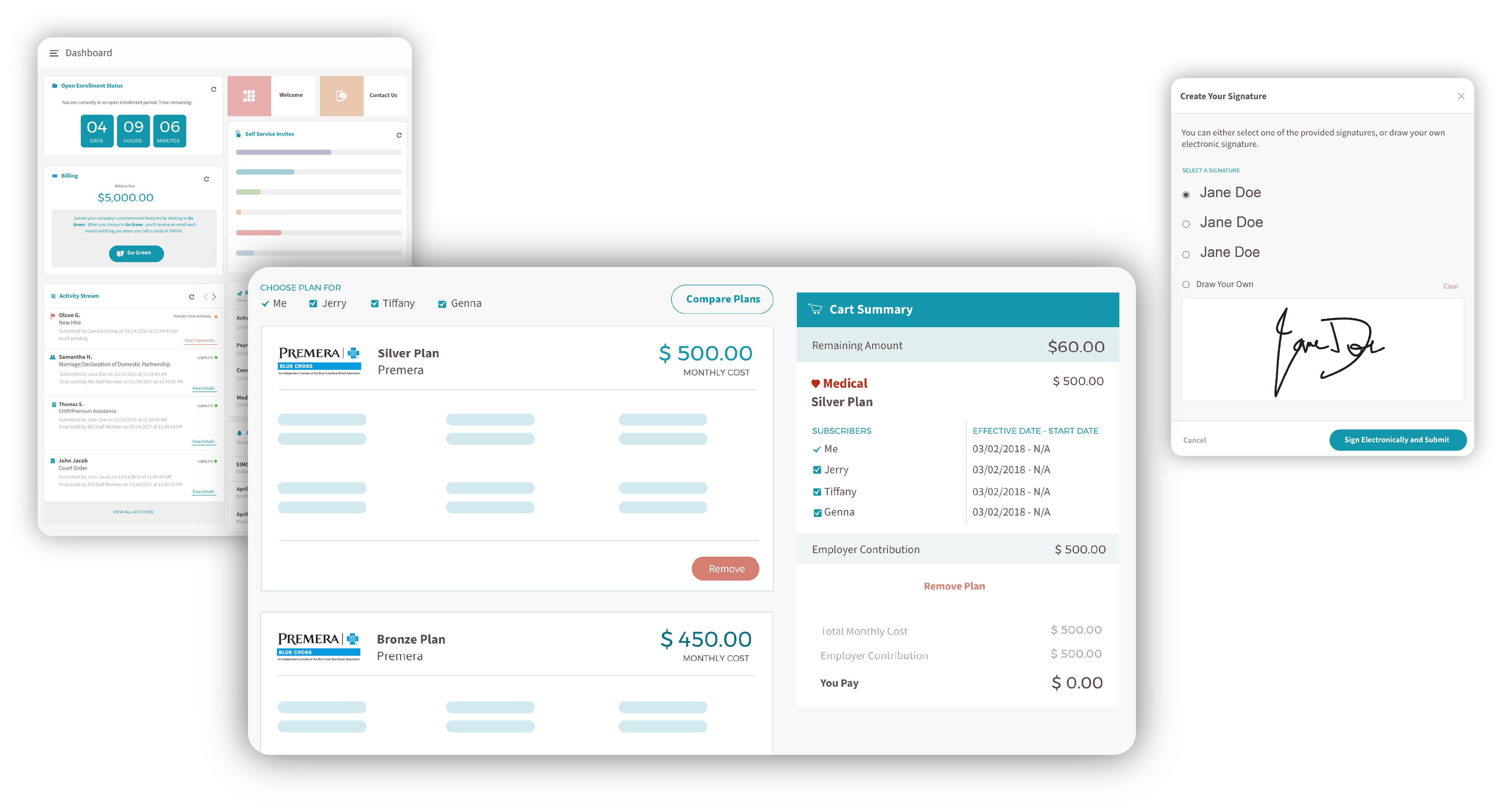
The result is a single, easy-to-read invoice — customized with your organization’s branding — and a reliable process that helps ensure every stakeholder receives the correct payment at the right time.
Key capabilities
Billing & invoicing
Client-specific branding and configuration
Consolidated invoices across all lines of coverage
Excel and PDF billing statements available through SIMON
Automated billing notifications
Payment management
EFT, ACH, and check payment options
Recurring and scheduled payment support
Premium reconciliation
Delinquency and collections management
Complexity support
Single- and multi-carrier product bundling (e.g., Small Group Self-Insured)
Support for complex or custom rate structures
Fee and commission schedule support
Individual billing and payments for COBRA members and retirees
Carrier + stakeholder alignment
Aggregated payment disbursement to brokers, general agents, carriers, and others
Accurate eligibility and premium submissions
Seamless alignment with SIMON’s enrollment and eligibility engine

Connected through the SIMON platform.
Integration with the SIMON platform keeps billing aligned with enrollment, eligibility, and data exchange across the benefits ecosystem. Consistent data flows support accuracy from invoicing through final disbursement without reconciliation gaps.
See SIMON in action.
Unlock fully consolidated invoicing with SIMON. Discover why organizations with complex benefits needs depend on Vimly for accurate, efficient billing with less manual effort.
